Note: This book quotes me approvingly, so this is not quite a disinterested review.
Cordelia Fine's Delusions of Gender is an engaging, entertaining and powerfully argued reply to the many authors - who range from the scientifically respectable to the less so - who've recently claimed to have shown biological sex differences in brain, mind and behaviour. Fine makes a strong case that the sex differences we see, in everything from behaviour to school achievements in mathematics, could be caused by the society in which we live, rather than by biology. Modern culture, she says, while obviously less sexist than in the past, still contains deeply entrenched assumptions about how boys and girls ought to behave, what they ought to do and what they're good at, and these - consciously or unconsciously - shape the way we are.
Fine makes a strong case that the sex differences we see, in everything from behaviour to school achievements in mathematics, could be caused by the society in which we live, rather than by biology. Modern culture, she says, while obviously less sexist than in the past, still contains deeply entrenched assumptions about how boys and girls ought to behave, what they ought to do and what they're good at, and these - consciously or unconsciously - shape the way we are.
Some of the Fine's targets are obviously bonkers, like Vicky Tuck, but for me, the most interesting chapters were those dealing in detail with experiments which have been held up as the strongest examples of sex differences, such as the Cambridge study claiming that newborn boys and girls differ in how much they prefer looking at faces as opposed to mechanical mobiles.
But Delusions is not, in Steven Pinker's phrase, saying we ought to return to "Blank Slatism", and it doesn't try to convince you that every single sex difference definately is purely cultural. It's more modest, and hence, much more believable: simply a reminder that the debate is still an open one.
Fine makes a convincing case (well, it convinced me) that the various scientific findings, mostly from the past 10 years, that seem to prove biological differences, are not, on the whole, very strong, and that even if we do accept their validity, they don't rule out a role for culture as well.
This latter point is, I think, especially important. Take, for example, the fact that in every country on record, men roughly between the ages of 16-30 are responsible for the vast majority of violent crimes. This surely reflects biology somehow; whether it's the fact that young men are physically the strongest people, or whether it's more psychological, is by the by.
But this doesn't mean that young men are always violent. In some countries, like Japan, violent crime is extremely rare; in other countries, it's tens of times more common; and during wars or other periods of disorder, it becomes the norm. Young men are always, relatively speaking, the most violent but the absolute rate of violence varies hugely, and that has nothing to do with gender. It's not that violent places have more men than peaceful ones.
Gender, in other words, doesn't explain violence in any useful way - even though there surely are gender differences. The same goes for everything else: men and women may well have, for biological reasons, certain tendencies or advantages, but that doesn't automatically explain (and it doesn't justify) all of the sex differences we see today; it's only ever a partial explanation, with culture being the other part.
Delusions of Gender
 13.50
13.50
 wsn
wsn
 Posted in
autism,
bad neuroscience,
books,
neurofetish
Posted in
autism,
bad neuroscience,
books,
neurofetish
In Dreams
 02.20
02.20
 wsn
wsn
 Freud's The Interpretation of Dreams is a very long book but the essential theory is very simple: dreams are thoughts. While dreaming, we are thinking about stuff, in exactly the same way as we do when awake. The difference is that the original thoughts rarely appear as such, they are transformed into weird images.
Freud's The Interpretation of Dreams is a very long book but the essential theory is very simple: dreams are thoughts. While dreaming, we are thinking about stuff, in exactly the same way as we do when awake. The difference is that the original thoughts rarely appear as such, they are transformed into weird images.
Only emotions survived unaltered. A thought about how you're angry at your boss for not giving you a raise might become a dream where you're a cop angrily chasing a bank robber, but not into one where you're a bank robber happily counting his loot. By interpreting the meaning of dreams, the psychoanalyst could work out what the patient really felt or wanted.
The problem of course is that it's easy to make up "interpretations" that follows this rule, whatever the dream. If you did dream that you were happily counting your cash after failing to get a raise, Freud could simply say that your dream was wish-fulfilment - you were dreaming of what you wanted to happen, getting the raise.
But hang on, maybe you didn't want the raise, and you were happy not to get it, because it supported your desire to quit that crappy job and find a better one...
Despite all that, since reading Freud I've found myself paying more attention to my dreams (once you start it's hard to stop) and I've found that his rule does ring true: emotions in dreams are "real", and sometimes they can be important reminders of what you really feel about something.
Most of my dreams have no emotions: I see and hear stuff, but feel very little. But sometimes, maybe one time in ten, they are accompanied by emotions, often very strong ones. These always seem linked to the content of the dream, rather than just being random brain activity: I can't think of a dream in which I was scared of something that I wouldn't normally be scared of, for example.
Generally my dreams have little to do with my real life, but those that do are often the most emotional ones, and it's these that I think provide insights. For example, I've had several dreams in the past six months about running; in every case, they were very happy ones.
Until several months ago I was a keen runner but I've let this slip and got out of shape since. While awake, I've regretted this, a bit, but it wasn't until I reflected on my dreams that I realized how important running was to me and how much I regret giving it up.
While awake, we're always thinking about things on multiple levels: we don't just want X, we think "I want X" (not the same thing), and then we go on to wonder "But should I want X?", "Why do I want X?", "What about Y, would that be better?", etc. Thoughts get piled up on top of one another: it's all very cluttered.
In a dream, most of the layers go silent, and the underlying feeling comes closer to the surface. The principle is the same, in many ways, as this.
But how do I know that feelings in dreams are the "real" ones? In most respects, dreams are less real than waking stuff: we dream about all kinds of crazy stuff. And even if we accept that dreams offer a window into our "underlying" feelings, who's to say that deeper is better or more real?
Well, "buried" feelings matter whenever they're not really buried. If a desire was somehow "repressed" to the point of having no influence at all, it might as well not exist. But my feelings about running were not unconscious as such - I was aware of them before I had these dreams - but I was "repressing" them, not in any mysterious sense, but just in terms of telling myself that it wasn't a big deal, I'd start again soon, I didn't have time, etc. The problem was that this "repression" was annoying, it was causing long-term frustration etc. In dreams, all of these mild emotions spanning several months were compressed into powerful feelings for the duration of the dream (a few minutes, although the dreams "felt like" they lasted hours).
The problem was that this "repression" was annoying, it was causing long-term frustration etc. In dreams, all of these mild emotions spanning several months were compressed into powerful feelings for the duration of the dream (a few minutes, although the dreams "felt like" they lasted hours).
Overall, I don't think it's possible or useful to interpret dreams as metaphorical representations in a Freudian sense (a train going into a tunnel = sex, or whatever). I suspect that dreams are more or less random activity in the visual and memory areas of the brain. But that doesn't mean they're meaningless: they're activity in your brain, so they can tell you about what you think and feel.
 Posted in
books,
freud,
mental health,
you
Posted in
books,
freud,
mental health,
you
I Feel X, Therefore Y
 02.40
02.40
 wsn
wsn
I'm reading Le Rouge et le Noir ("The Red and the Black"), an 1830 French novel by Stendhal...
In Paris, the nature of [her] attitude towards [him] would have very quickly become plain - but in Paris, love is an offspring of the novels. In three or four such novels, or even in a couplet or two of the kind of song they sing at the Gymnase, the young tutor and his shy mistress would have found a clear explanation of their relations with each other. Novels would have traced out a part for them to play, given them a model to imitate.
Notice that his claim is not that novels create entirely new emotions. The two characters had feelings for each other despite never having read any. Novels suggest roles to play and models to follow: in other words, they provide interpretations as to what emotions mean and expectations as to what behaviours they lead to. You feel that, therefore you'll do this.
This bears on many things that I've written about recently. Take the active placebo phenomenon. This refers to cases in which a drug creates certain feelings, and the user interprets these feelings as meaning that "the drug is working", so they expect to improve, which leads them to feel better and behave as if they are getting better.
As I said at the time, active placebos are most often discussed in terms of drug side effects creating the expectation of improvement, but the same thing also happens with real drug effects. Valium (diazepam) produces a sensation of relaxation and reduces anxiety as a direct pharmacological effect but if someone takes it expecting to feel better, this will also drive improvement via expectation: the Valium is working, I can cope with this.
The same process can be harmful, though, and this may be even more common. The cognitive-behavioural theory of recurrent panic attacks is that they're caused by vicious cycles of feelings and expectations. Suppose someone feels a bit anxious, or notices their heart is racing a little. They could interpret that in various ways. They might write it off and ignore it, but they might conclude that they're about to have a panic attack.
If so, that's understandably going to make them more anxious, because panic is horrible. Anxiety causes adrenaline released, the heart beats ever faster etc., and this causes yet more anxiety until a full-blown panic attack occurs. The more often this happens, the more they come to fear even minor symptoms of physical arousal because they expect to suffer panic. Cognitive behavioural therapy for panic generally consists of breaking the cycle by changing interpretations, and by gradual exposure to physical symptoms and "panic-inducing" situations until they no longer cause the expectation of panic.
 This also harks back to Ethan Watters' book Crazy Like Us which I praised a few months back. Watters argued that much mental illness is shaped by culture in the following way: culture tells us what to expect and how people behave when they feel distressed in certain ways, and thus channels distress into recognizable "syndromes" - a part to play, a model to imitate, though probably quite unconsciously. The most common syndromes in Western culture can be found in the DSM-IV, but this doesn't mean that they exist in the rest of the world.
This also harks back to Ethan Watters' book Crazy Like Us which I praised a few months back. Watters argued that much mental illness is shaped by culture in the following way: culture tells us what to expect and how people behave when they feel distressed in certain ways, and thus channels distress into recognizable "syndromes" - a part to play, a model to imitate, though probably quite unconsciously. The most common syndromes in Western culture can be found in the DSM-IV, but this doesn't mean that they exist in the rest of the world.Like Stendhal's, this theory does not attempt to explain everything - it assumes that there are fundamental feelings of distress - and I do not think that it explains the core symptoms of severe mental illness such as bipolar disorder and schizophrenia. But people with bipolar and schizophrenia have interpretations and expectations just like everyone else, and these may be very important in determining long-term prognosis. If you expect to be ill forever and never have a normal life, you probably won't.
 Posted in
books,
crazylikeus,
mental health,
philosophy,
placebo,
you
Posted in
books,
crazylikeus,
mental health,
philosophy,
placebo,
you
Fingers
 03.10
03.10
 wsn
wsn
 How many fingers do you have?
How many fingers do you have?
10, obviously, unless you've been the victim of an accident or a birth defect. Everyone knows that. You count up to ten on your fingers, for one thing.
But look at your left hand - how many fingers are on it? Little finger, ring finger, middle finger, first finger... thumb. So that's 4. But then we'd only have 8 fingers, and we all know we have 10. Unless the thumb is a finger, but is it?
Hmm. Hard to say. Wikipedia has some interesting facts about this question, and on Google if you start to type in "is the thumb", the top suggested search terms are all about this issue. It's a tricky one. People don't seem to know for sure.
But does that mean there's any real mystery about the thumb? No - we understand it as well as any other part of the body. We know all about the bones and muscles and joints and nerves of the thumb, we know how it works, what it does, even its evolutionary history (see The Panda's Thumb by Steven J Gould, still one of the greatest popular science books ever.) Science has got thumbs covered.
The mystery is in the English language, which isn't quite clear on whether the word "finger" encompasses the human thumb; for some purposes it does, i.e. we have 10 fingers, but for other purposes it probably doesn't, although even English speakers seem to be in two minds about the details (see Google, above).
Notice that although the messiness seems to focus on the thumb, the word "thumb" is perfectly clear. The ambiguity is rather in the word "finger", which can mean either any of the digits of the hand, or, the digits of the hand with three joints. Take a look at your hand again and you'll notice that your thumb lacks a joint compared to the fingers; something I must admit I'd forgotten until Wikipedia reminded me.
Yet it would be very easy to blame the thumb for the confusion. After all, the other 4 fingers are definitely fingers. The fingers are playing by the rules. Only the thumb is a troublemaker. So it comes as somewhat of a surprise to realize that it's the fingers, not the thumb, that are the problem.
It's important to bear in this in mind when thinking about psychiatry, because psychiatry has an awful lot of confusion, and a lot of it can be traced back to ambiguous terms. Take, for example, the question of whether X "is a mental illness". Is addiction a mental illness, or a choice? Is mild depression a mental illness, or a normal part of life? Is PTSD a mental illness, or a normal reaction to extreme events? Is... I could go on all day.
The point is that you will never be able to answer these questions until you stop focussing on the particular case and first ask, what do I mean by mental illness? If you can come up with a single, satisfactory definition of mental illness, all the edge cases will become obvious. But at present, I don't think anyone really knows what they mean by this term. I know I don't, which is why I try to avoid using it, but often I do still use it because it seems to be the most fitting phrase.
It might seem paradoxical to use a word without really knowing what it means, but it isn't, because being able to use a word is procedural knowledge, like riding a bike. The problem is that many of our words have confusion built-in, because they're ambiguous. We can all use them, but that means we're all risking confusing each other, and ourselves. When this gets serious enough the only solution is to stop using the offending word and create new, unambiguous ones. With "finger", it's hardly a matter of life or death. With "mental illness", however, it is.
 Posted in
books,
mental health,
philosophy
Posted in
books,
mental health,
philosophy
Carlat's Unhinged
 04.45
04.45
 wsn
wsn
Well he's not. Actually, I haven't met him, so it's always possible. But what he certainly has done is written a book called Unhinged: The Trouble with Psychiatry. Daniel Carlat's best known online for the Carlat Psychiatry Blog and in the real world for the Carlat Psychiatry Report. Unhinged is his first book for a general audience, though he's previously written several technical works aimed at doctors. It comes hot on the heels of a number of other recent books offering more or less critical perspectives on modern psychiatry, notably these ones.
Daniel Carlat's best known online for the Carlat Psychiatry Blog and in the real world for the Carlat Psychiatry Report. Unhinged is his first book for a general audience, though he's previously written several technical works aimed at doctors. It comes hot on the heels of a number of other recent books offering more or less critical perspectives on modern psychiatry, notably these ones.
Unhinged offers a sweeping overview of the whole field. If you're looking for a detailed examination of the problems around, say, psychiatric diagnosis, you'd do well to read Crazy Like Us as well. But as an overview it's a very readable and comprehensive one, and Carlat covers many topics that readers of his blog, or indeed of this one, would expect: the medicalization of normal behaviour, to over-diagnosis, the controversy over pediatric psychopharmacology, brain imaging and the scientific state of biological psychiatry, etc.
Carlat is unique amongst authors of this mini-genre, however, in that he is himself a practising psychiatrist, and moreover, an American one. This is important, because almost everyone agrees that to the extent that there is a problem with psychiatry, American psychiatry has it worst of all: it's the country that gave us the notorious DSM-IV, where drugs are advertised direct-to-the-consumer, where children are diagnosed with bipolar and given antipsychotics, etc.
So Carlat is well placed to report from the heart of darkness and he doesn't disappoint, as he vividly reveals how dizzying sums of drug company money sway prescribing decisions and even create diseases out of thin air. His confessional account of his own time as a paid "representative" for the antidepressant Effexor (also discussed in the NYT), and of his dealings with other reps - the Paxil guy, the Cymbalta woman - have to be read to be believed. We're left with the inescapable conclusion that psychiatry, at least in America, is institutionally corrupt.
Conflict of interest is a tricky thing though. Everyone in academia and medicine has mentors, collaborators, people who work in the office next door. The social pressure against saying or publishing anything that explicitly or implicitly criticizes someone else is powerful. Of course, there are rivalries and controversies, but they're firmly the exception.
The rule is: don't rock the boat. And given that in psychiatry, all but a few of the leading figures have at least some links to industry, that means everyone's in the same boat with Pharma, even the people who don't, personally, accept drug company money. I think this is often overlooked in all the excitement over individual scandals.
For all this, Carlat is fairly conservative in his view of psychiatric drugs. They work, he says, a lot of the time, but they're rarely the whole answer. Most people need therapy, too. His conclusion is that psychiatrists need to spend more time getting to know their patients, instead of just handing out pills and then doing a 15 minute "med check" - a great way of making money when you're getting paid per patient (4 patients per hour: ker-ching!), but probably not a great way of treating people.
In other words, psychiatrists need to be psychotherapists as well as psychopharmacologists. It's not enough to just refer people to someone else for the therapy: in order to treat mental illness you need one person with the skills to address both the biological and the psychological aspects of the patient's problems. Plus, patients often find it frustrating being bounced back and forth between professionals, and it's a recipe for confusion ("My psychiatrist says this but my therapist says...")
As he puts it, for a psychiatrist, the years in medical school spent delivering babies and dissecting kidneys are rarely useful. So there's no reason why a therapist can't learn the necessary elements of psychopharmacology - which drugs do what, how to avoid dangerous drug interactions - in say one or two years.
Such a person would be at least as good as a psychiatrist at providing integrated pills-and-therapy care. In fact, he says, an even better option would be to design an entirely new type of training program to create such "integrated" mental health professionals from the ground up - neither doctors nor therapists but something combining the best aspects of both.
There does seem to be a paradox here, however: Carlat has just spent 200 pages explaining how drug companies distort the evidence and bribe doctors in order to push their latest pills at people, many of whom either don't need medication or would do equally well with older, much cheaper drugs. Now he's saying that more people should be licensed to prescribe the same pills? Whose side is he on?
In fact, Carlat's position is perfectly coherent: his concern is to give patients the best possible care, which is, he thinks, combined medication and therapy. So he is not "anti" or "pro-medication" in any simple sense. But still, if psychiatry has been corrupted by drug company money, what's to stop the exact same thing happening to psychologists as soon as they got the ability to prescribe?
I think the answer to this can only be that we must first cut the problem off at its source by legislation. We simply shouldn't allow drug companies the freedom to manipulate opinion in the way that they do. It's not inevitable: we can regulate them. The US leads the world in some areas: since 2007, all clinical trials conducted in the country must be pre-registered, and the results made available on a public website, clinicaltrials.gov.
The benefits, in terms of keeping drug manufacturer's honest, are far too many to explain here. Other places, like the European Union, are just starting to follow suit. But America suffers from a split personality in this regard. It's also one of the only countries to allow direct-to-consumer drug advertising, for example. Until the US gets serious about restraining Pharma influence in all its forms, giving more people prescribing rights might only aggravate the problem.
 Posted in
antidepressants,
blogging,
books,
mental health,
politics
Posted in
antidepressants,
blogging,
books,
mental health,
politics
DSM-V, a Prenatal Health Check
 04.00
04.00
 wsn
wsn
Last month the proposed draft of the 5th edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-V) came out.
 In my post at the time I was pretty critical of several aspects of the new DSM. Many many other blogs have discussed DSM-V, as have older media. As you'd expect with such a complex and controversial issue as psychiatric diagnosis, opinions have varied widely, but one thing stands out: people are debating this. Everyone's got something to say about it, professionals and laypeople.
In my post at the time I was pretty critical of several aspects of the new DSM. Many many other blogs have discussed DSM-V, as have older media. As you'd expect with such a complex and controversial issue as psychiatric diagnosis, opinions have varied widely, but one thing stands out: people are debating this. Everyone's got something to say about it, professionals and laypeople.Debate is usually thought to be healthy, but I think in this case, it's a very bad sign for DSM-V. The previous editions, like DSM-IV, were presented to the world as a big list of mental disorders carrying the authority of the American Psychiatric Association. That's why people called the DSM the Bible of psychiatry - it was supposedly revealed truth as handed down by a consensus group of experts. If not infallible, it was at least something to take note of. There have always been critics of the DSM, but until recently, they were the underdogs, chipping away at an imposing edifice.
But DSM-V won't be imposing. People are criticizing it before it's been finalized, and even bystanders can see that there's really no consensus on many important issues. The very fact that everyone's discussing the proposed changes to the Manual is also telling: if the DSM is a Bible, why does it need to be revised so often?
My prediction is that when DSM-V does arrive (May 2013 is the current expected birth date) , it will be a non-event. By then the debates will have happened. I suspect that few researchers are going to end up deciding to invest their time, money and reputation in the new disorders added in DSM-V. Why study "temper regulation disorder with dysphoria" (TDDD) when it was controversial before it even officially existed? Despite the shiny new edition, we may be using DSM-IV for all intents and purposes for a long time to come.
 Posted in
books,
media,
mental health
Posted in
books,
media,
mental health
DSM-V: Change We Can Believe In?
 02.25
02.25
 wsn
wsn
So the draft of DSM-V is out. If, as everyone says, the Diagnostic and Statistical Manual is the Bible of Psychiatry, I'm not sure why it gets heavily edited once every ten years or so. Perhaps the previous versions are a kind of Old Testament, and only the current one represents the New Revelation from the gods of the mind?
If, as everyone says, the Diagnostic and Statistical Manual is the Bible of Psychiatry, I'm not sure why it gets heavily edited once every ten years or so. Perhaps the previous versions are a kind of Old Testament, and only the current one represents the New Revelation from the gods of the mind?
Mind Hacks has an excellent summary of the proposed changes. Bear in mind that the book won't be released until 2013. Some of the headlines:
- Asperger's Syndrome is out - everyone's going to have an "autistic spectrum disorder" now.
- Personality Disorders are out - kind of. In their place, there's 5 Personality Disorder Types, each of which you can have to varying degrees, and also 6 Personality Traits, each of which you can have to varying degrees.
- Hypoactive Sexual Desire Disorder - the disease which failed-antidepressant-turned-aphrodisiac flibanserin is supposed to treat - is out, to be replaced by Sexual Interest and Arousal Disorder.
- Binge Eating Disorder, Hypersexuality Disorder, and Gambling Addiction are in. Having Fun is not a disorder yet, but that's on the agenda for DSM-VI.
Excitingly, "dimensional assessments" have been added... but only in a limited way. Some people have long argued that having categorical diagnoses - "schizophrenia", "bipolar disorder", "major depression" etc. - is a mistake, since it forces psychiatrists to pigeon-hole people, and that we should stop thinking in terms of diagnoses and just focus on symptoms: if someone's depressed, say, then treat them for depression, but don't diagnose them with "major depressive disorder".
DSM-V hasn't gone this far - the categorical diagnoses remain in most cases (the exception is Personality Disorders, see above). However, new dimensional assessments have been proposed, which are intended to complement the diagnoses, and some of them will be "cross-cutting" i.e. not tied to one particular diagnosis. See for example here for a cross-cutting questionnaire designed to assess common anxiety, depression and substance abuse symptoms.
Finally, the concept of "mental disorder" is being redefined. In DSM-V a mental disorder is (drumroll)...
A. A behavioral or psychological syndrome or pattern that occurs in an individualThe main change here is that now it's all about "psychobiological dysfunction", whereas in DSM-IV, it was about "behavioral, psychological, or biological dysfunction". Hmm. I am not sure what this means, if anything.
B. The consequences of which are clinically significant distress (e.g., a painful symptom) or disability (i.e., impairment in one or more important areas of functioning)
C. Must not be merely an expectable response to common stressors and losses...
D. That reflects an underlying psychobiological dysfunction
E. That is not primarily a result of social deviance or conflicts with society
But read on, and we find something rather remarkable...
J. When considering whether to add a mental/psychiatric condition to the nomenclature, or delete a mental/psychiatric condition from the nomenclature, potential benefits (for example, provide better patient care, stimulate new research) should outweigh potential harms (for example, hurt particular individuals, be subject to misuse)This all sounds very nice and sensible. Diagnoses should be helpful, not harmful, right?
No. Diagnoses should be true. The whole point of the DSM is that it's supposed to be an accurate list of the mental diseases that people can suffer from. The diagnoses are in there because they are, in some sense, real, objectively-existing disorders, or at least because the American Psychiatric Association thinks that they are.
This seemingly-innocuous paragraph seems to be an admission that, in fact, disorders are added or subtracted for reasons which have little to do with whether they really, objectively exist or not. This is what's apparently happened in the case of Temper Dysregulation Disorder with Dysphoria (TDDD), a new childhood disorder.
TDDD has been proposed in order to reduce the number of children being diagnosed with pediatric bipolar disorder. The LA Times quote a psychiatrist on the DSM-V team:
The diagnosis of bipolar [in children] "is being given, we believe, too frequently," said Dr. David Shaffer, a member of the work group on disorders in childhood and adolescence. In reality, when such children are tracked into adulthood, very few of them turn out to be bipolar, he said.And the DSM-V website has a lengthy rationale for TDDD, to the same effect.
Now, many people agree that pediatric bipolar is being over-diagnosed. As I've written before, pediatric bipolar was considered to be a vanishingly rare disease until about 10 years ago, it still is pretty much everywhere outside the USA.
So we can all sympathize with the sentiment behind TDDD - but this is fighting fire with fire. Is the only way to stop kids getting one diagnosis, to give them another one? Should we really be creating diagnoses for more or less "strategic" purposes? When the time comes for DSM-VI, and the fashion for "pediatric bipolar" has receded, will TDDD get deleted as no longer necessary? What will happen to all the "TDDD" kids then?
Can't we just decide to diagnose people less? Apparently, that would be a rather too radical change...
 Posted in
autism,
books,
mental health,
science
Posted in
autism,
books,
mental health,
science
Dope, Dope, Dopamine
 14.10
14.10
 wsn
wsn
When you smoke pot, you get stoned.
In Central nervous system effects of haloperidol on THC in healthy male volunteers, Liem-Moolenaar et al tested whether an antipsychotic drug would modify the psychoactive effects of Δ9-THC, the main active ingredient in marijuana. They took healthy male volunteers, who had moderate experience of smoking marijuana, and gave them inhaled THC. They were pretreated with 3 mg haloperidol, or placebo.
They found that haloperidol reduced the "psychosis-like" aspects of the marijuana intoxication. However, it didn't reverse the effects of THC of cognitive performance, the sedative effects, or the user's feelings of "being high".
This makes sense, if you agree with the theory that the psychosis-like effects of THC are related to dopamine. Like all antipsychotics, haloperidol blocks dopamine D2 receptors, and increased dopamine transmission has long been implicated in psychosis; some studies have found that THC causes increased dopamine release in humans (although others have not.)
Heavy marijuana use probably raises the risk of psychotic illnesses, like schizophrenia, although this is still a bit controversial, but it's accepted that some people do experience psychotic-type symptoms while stoned. So Liem-Moolenaar et al's conclusion that "psychotic-like effects induced by THC are mediated by dopaminergic systems" while the other aspects of being stoned are mediated by other brain systems, is not unreasonable, and this study is a nice example of the 'pharmacological dissection' of drug effects.
Still, like most papers of this kind, this leaves me wanting to know more about the subjective effects experienced by the volunteers. What did it feel like to get stoned on haloperidol? The paper tells us that
THC caused a significant increase of 2.5 points in positive PANSS, which was significantly reduced by 1.1 points after pre-treatment with haloperidol... Haloperidol completely reversed THC-induced increases in ‘delusions’ and ‘conceptual disorganization’ and almost halved the increase in ‘hallucinatory behaviour’. Although not statistically significant, haloperidol seemed to increase the items ‘conceptual disorganization’, ‘suspiciousness/persecution’ and ‘hostility’ compared with placebo.The PANSS being a scale used to rate someone's "psychotic symptoms". On the other hand haloperidol had no significant effect on the users' self-rated Visual Analogue Scales (VAS) scores for things like "altered external perception" and "feeling high".
 But surely the haloperidol must have changed what it felt like in some way. It must have changed how people thought, felt, perceived, heard, and so forth. These kinds of rating scales are useful for doing statistics with, but they can no more capture the full depth of human experience than a score out of 5 stars substitutes for a full Roger Ebert movie review.
But surely the haloperidol must have changed what it felt like in some way. It must have changed how people thought, felt, perceived, heard, and so forth. These kinds of rating scales are useful for doing statistics with, but they can no more capture the full depth of human experience than a score out of 5 stars substitutes for a full Roger Ebert movie review.This matters, because it's not clear whether haloperidol really reduced "psychosis-like experiences", or whether it just sedated people to the extent that they were less likely to talk about them. In other words, its not clear whether the scores on the rating scales changed in "specific" or a "non-specific" way. This is no criticism of Liem-Moolenaar, though, because it's a general problem in psychopharmacology. For example, a sleeping pill could reduce your score on most depression rating scales, even if it had no effect on your mood, because insomnia is a symptom of depression.
There are various ways to try to work around these issues, but ultimately I suspect that there's no substitute for personal experience, with direct observation of other people taking the drugs coming second, and rating scales a distant third. Of course, direct observation is unsystematic, and prone to bias, and few would say it was practical for psychopharmacologists to go around drugging themselves and each other... but life is more than a series of numbers.
Link: On Being Stoned (1971) by Charles Tart is a classic book which used a very detailed questionnaire to investigate what it's like to be stoned, although the methodology was hardly rigorous.
 Posted in
books,
CNR1,
drugs,
marijuana,
mental health,
papers,
schizophrenia
Posted in
books,
CNR1,
drugs,
marijuana,
mental health,
papers,
schizophrenia
Crazy Like Us
 09.30
09.30
 wsn
wsn
You've probably heard about Crazy Like Us, the new book by Urban Tribes author Ethan Watters. But you probably haven't bought it yet. You really should. Crazy Like Us is a vivid, humane, and thought-provoking examination of "the globalization of the American psyche" - the process by which, slowly but surely, the world has adopted America's way of thinking about mental illness.
Crazy Like Us is a vivid, humane, and thought-provoking examination of "the globalization of the American psyche" - the process by which, slowly but surely, the world has adopted America's way of thinking about mental illness.
The key to the American approach is the 844-page Diagnostic and Statistical Manual of the American Psychiatric Association - the DSM, or as the saying goes, the Bible of psychiatry. The heart of the DSM is a long list of disorders, each with a code number, and each with an accompanying list of symptoms: Major Depressive Disorder (296.2), Post-Traumatic Stress Disorder (309.81), Schizophrenia (295.90), etc. The DSM is more than just a catalogue of names and numbers, however; it's part a conceptual system, a way of deciding what kind of feelings and behaviours are normal, and which are pathological; it's almost a philosophy of life.
On the most straightforward level, Crazy Like Us is the story of how, over the past 20 years, this system has gone from being American to international, displacing the ways of thinking found in other countries and cultures. In four chapters, Watters describes the rise of anorexia in Hong Kong, PTSD in Sri Lanka following the 2004 tsunami, schizophrenia in Madagascar, and major depressive disorder in Japan.
This much is plain fact. The DSM is now the internationally-recognized standard for psychiatric diagnosis; almost all academic papers in psychiatry make use of the American criteria, or the extremely similar ICD-10. What's interesting, however, is Watters' account of how the DSM spread so quickly to other countries, displacing what were - in many cases - equally rich and complex local vocabularies of distress and disorder.
In the case of Japan, Watters' answer is simple: the big drug companies, in the hopes of opening a new market for SSRI antidepressants, promoted the concept of clinical depression as a common ailment, through campaigns in the Japanese media. (Japan did have an "indigenous" concept of depression, utsubyo, but it was seen as a rare, serious disease, like schizophrenia.)
But in "developing" countries, such as Sri Lanka, the picture is rather more complex. Sri Lankans were eager to learn from the West about mental illness because of their respect for Western science and technology. Americans can put people into space - surely, they know a lot about everything, including medicine, including psychiatry.
Yet there's another level to the story of Crazy Like Us, a more interesting and more controversial one. Watters' argues that the globalization of the American way of thinking has actually changed the nature of "mental illness" around the world. As he puts it:
In the process of teaching the rest of the world to think like us, we’ve been exporting our Western “symptom repertoire” as well. That is, we’ve been changing not only the treatments but also the expression of mental illness in other cultures.

The historian of psychiatry, Edward Shorter, has written of how, in late 19th century Europe, people (mostly women) were said to be especially prone to suffering from "hysterical paralysis", but every time and place has its own shared "symptom repertoire". Culture does not just create symptoms out of thin air - there has to be some kind of underlying stress. As Watters puts it
We can become psychologically unhinged for many reasons that are common to all, like personal traumas, social upheavals or biochemical imbalances in our brains. ... Whatever the trigger, however, the ill individual and those around him invariably rely on cultural beliefs and stories to understand what is happening.
The idea that America has exported not just concepts of illness, but illnesses themselves, is a provocative one. Is it true? Commentators have pointed out that Watters' explanation of the rise of anorexia in Hong Kong is rather simplistic. There were many social and cultural changes going on during the 1990s, most of which had nothing to do with the DSM. How do we know that increasing media promotion of dieting, and the fashion for thinness, wasn't also important? In truth, we don't, but I do not think that Watters' argument requires psychiatry to be the only force at work.
If our way of thinking about mental illness is as culturally bound as any other, then our own "psychiatric disorders" are no more eternal and objectively real than those Malaysian syndromes like amok, episodes of anger followed by amnesia, or koro, the fear the that ones genitals are shrinking away.
In other words, maybe patients with "anorexia", "PTSD" and perhaps "schizophrenia" don't "really" have those things at all - at least not if these are thought of as objectively-existing diseases. In which case, what do they have? Do they have anything? And what are we doing to them by diagnosing and treating them as if they did?
Watters' does not discuss such questions; I think this was the right choice, because a full exploration of these issues would fill at least one book in itself. But here are a few thoughts:
First, the most damaging thing about the globalization of Western psychiatric concepts is not so much the concepts themselves, but their tendency to displace and dissolve other ways of thinking about suffering - whether they be religious, philosophical, or just plain everyday talk about desires and feelings. The corollary of this, in terms of the individual Western consumer of the DSM, i.e. you and me, is the tendency to see everything through the lens of the DSM, without realizing that it's a lens, like a pair of glasses that you've forgotten you're even wearing. So long as you keep in mind that it's just one system amongst others, a product of a particular time and place, the DSM is still useful.
Second, if it's true that how we conceptualize illness and suffering affects how we actually feel and behave, then diagnosing or narrativizing mental illness is an act of great importance, and potentially, great harm. We currently spend billions of dollars researching major depressive disorder and schizophrenia, but very little on investigating "major depressive disorder" and "schizophrenia" as diagnoses. Maybe this is an oversight.
Finally, if much "mental illness" is an expression of fundamental distress shaped by the symptom pool of a particular culture, then we need to first map out and understand the symptom pool, and the various kinds of distress, in order to have any hope of making sense of what's going on in any individual on a psychological, social or neurobiological level. To put it another way, you need to understand people before you can understand psychiatry. After reading Crazy Like Us, I think I understand both a little bit better, and I strongly recommend it.
Links:
- Ethan Watters' Crazy Like Us blog.
- The Americanization of Mental Illness, Watters' much-read NYT article which is a fine summary of the book's argument, but being so short, misses much of the human detail which make Crazy Like Us so interesting, in particular when Watters is writing about the response of PTSD experts to the 2004 tsunami, and the life of a Madagascan woman with schizophrenia and her family.
- Exporting American Mental Illness, an excellent discussion of the article over at Neuroanthropology.
- Did Antidepressants Depress Japan? A 2004 article on the Japanese antidepressants and depression story.
 Posted in
1in4,
antidepressants,
books,
crazylikeus,
media,
mental health,
you
Posted in
1in4,
antidepressants,
books,
crazylikeus,
media,
mental health,
you
ECT in Nixonland
 05.45
05.45
 wsn
wsn
 I've just finished Nixonland, Rick Perlstein's history of the 1960s. Some things I learned: Richard Nixon was a genius, albeit an evil one; the 1960s never ended; Rick Perlstein is my new favourite political author.
I've just finished Nixonland, Rick Perlstein's history of the 1960s. Some things I learned: Richard Nixon was a genius, albeit an evil one; the 1960s never ended; Rick Perlstein is my new favourite political author.
The book also reminded me of a sad episode in the history of psychiatry.
George McGovern ran against Nixon as the Democratic candidate for President in 1972. He was essentially the Obama of the 60s generation: unashamedly liberal and intellectual, he unseated the "established" candidate, Hubert Humphrey, to clinch the Democrat's nomination after a bitter primary campaign thanks to his idealistic young grass-roots.
McGovern had difficulty choosing his vice-presidential running mate, and eventually chose a little-known Senator from Missouri, Thomas Eagleton (left in the photo). It seemed a safe enough choice. Until Eagleton's first press conference.
Eagleton revealed that he'd been treated in a psychiatric hospital for "exhaustion" - everyone knew he meant clinical depression - three times, and that he had received electroconvulsive therapy twice. McGovern hadn't known this when he picked him.
From there it was all downhill. McGovern initially said he backed Eagleton "1000%". But to some, the idea of putting someone who'd had shock therapy a heartbeat away from the Presidency was unacceptable, and after two weeks of gossip, McGovern dropped him from the ticket.
Perlstein notes that this move wrecked McGovern's image as the idealistic and authentic alternative to politics-as-usual. Polls showed that Americans overwhelmingly trusted Nixon over McGovern, even as the facts about Watergate were emerging. Nixon won a landslide.
 Posted in
books,
history,
mental health
Posted in
books,
history,
mental health
Book: Deep Brain Stimulation
 12.06
12.06
 wsn
wsn
 Jamie Talan's Deep Brain Stimulation: A New Treatment Shows Promise In The Most Difficult Cases is the first book to offer a popular look at DBS, one of the more exciting emerging treatments in neurology and psychiatry.
Jamie Talan's Deep Brain Stimulation: A New Treatment Shows Promise In The Most Difficult Cases is the first book to offer a popular look at DBS, one of the more exciting emerging treatments in neurology and psychiatry.
Deep Brain Stimulation is not a textbook and the depth of scientific detail is kept pretty low, but the breadth of the material is good. Talan reviews the many kinds of disorders for which DBS has been trialled, from the early 1990s when it was used in Parkinson's disease up to the past five years where it's been tried for everything from epilepsy, depression and Tourette's Syndrome up to lifting patients out of persistent vegetative states (maybe).
Unfortunately, Talan doesn't discuss the controversial history of the first era of human brain stimulation, including the morally murky work of Robert G. Heath at Tulane University in the 1960s. She mentions Tulane once in passing but more detail would have been welcome, if only because it's a rather spicy tale.
The book's most engaging passages are the stories of individual patients. There's the man with Parkinson's who experienced amazing benefits from DBS, and who was so keen to keep them that he didn't tell doctors about the infection which developed a few weeks after surgery, in case they took the electrode out. After literally keeping the infected site under his hat for a few days, it progressed to a brain abscess, and he nearly died. Happily, he not only survived but was able to get the electrodes reimplanted.
Then there's the most moving case, that of the woman suffering from severe OCD and depression, who was given experimental DBS for the former condition. She died by suicide several months later, but said in her suicide note that the DBS had worked - her OCD symptoms were gone. Her depression was as bad as ever, though, and this is what led her to suicide. She wanted people to know that deep brain stimulation helped her, and didn't want her death to go down in the records as a mark against it.
The precursor to DBS was ablative neurosurgery - destroying particular parts of the brain in order to relieve symptoms. Talan describes its use in movement disorders such as Parkinson's, but she glosses over the history of "psychosurgery", the use of surgery to treat mental illness. People using DBS in psychiatry often prefer not to talk about psychosurgery - it's not exactly good PR. But clearly it is relevant. For all its faults, psychosurgery did seem to help some patients, which is why it's still used today in rare cases, although DBS may soon replace it.
DBS for depression and OCD usually target the same prefrontal white matter pathways that psychosurgery severed, so scientifically, psychosurgery has lessons for DBS. The ethical issues overlap too. Although DBS is reversible, unlike brain lesioning, it carries the same risks of serious complications like infection or brain bleeding. And there's the same question of whether seriously mentally ill people can give informed consent.
The book's strongest chaper is the last, which covers the ethical and practical difficulties of DBS. The danger is that enthusiastic doctors with no experience of the procedure, encouraged by the tales from other hospitals, might start doing it inappropriately. There's also a risk that patients or their families might volunteer for DBS prematurely or have impossibly high expectations. The initial results have been very promising, but there have been no large placebo-controlled trials so far (except in some movement disorders). And even with the best surgeons, in most disorders the response rate seems to hover around the 50-60% mark. Talan warns that DBS risks being a victim of its own hype. That's an important message.
 Posted in
books,
dbs,
mental health
Posted in
books,
dbs,
mental health
The British are Incredibly Sad
 11.37
11.37
 wsn
wsn
 Or so says Oliver James(*) on this BBC radio show in which he also says things like "I absolutely embraces the credit crunch with both arms".
Or so says Oliver James(*) on this BBC radio show in which he also says things like "I absolutely embraces the credit crunch with both arms".
Oliver James is a British psychologist best known for his theory of "Affluenza". This is his term for unhappiness and mental illness caused, he thinks, by an obsession with money, status and possessions. Affluenza, James thinks, is especially prevanlent in English-speaking countries, because we're more into free-market capitalism than the people of mainland Europe. In fact, he regularly makes the claim that we in Britain, the U.S., Australia etc. are today twice as likely to be mentally ill as "the Europeans". This is because rates of mental illness supposedly surged in the English-speaking world due to 1980s Reagan/Thatcher free market policies. Hence why he welcomes the current economic unpleasantness.
Were all of this true, it would be incredibly important. Certainly important enough to justify writing three books about it and seemingly endless articles for the Guardian. But is it true? Well, this is Neuroskeptic, so you can probably guess. Also, bear in mind that James is someone who is on record as thinking that
[The Tears for Fears song] Mad World. With the chilling line "The dreams in which I'm dying are the best I've ever had", in some respects it is up there with TS Eliot's Prufrock as a poetic account of bourgeois despair.Obviously poetic taste is entirely subjective etc., but honestly.
Anyway, where did James get the twice-as-bad-as-Europe (or, in some articles, three times as bad) idea from? He says the World Health Organization. Presumably he is referring to one of the World Health Organization's World Mental Health Surveys, such as the analysus presented in this JAMA paper.
At first glance, you can see what he means. This paper reports that the % of people reporting suffering from at least one mental illness over the last year was far higher in the US (26.4%) than in say Italy (8.2%), or Nigeria (4.7%). But on closer inspection, even this data includes some incongruous numbers. Why is Beijing (9.1%) twice as bad as Shanghai (4.3%)? Worse, why does France have a rate of 18.4% while across the border in Germany it's just 9.1%? Are the French twice as materialistic as the Germans? The answer, of course, is that these numbers are more complicated than they appear. In fact, if you believe those figures at face value, you are...well, you're probably Oliver James.
These numbers come from structured interviews, conducted by trained lay researchers, of a random sample of the population. In other words, some guy asked some random people a series of fairly personal questions, reading them off a list, and if they said "Yes" to questions like "Have you ever in your life had a period lasting several days or longer when most of the day you felt sad, empty or depressed?" they might get a tick for "depression". We know this because the interviews used the WHO-CIDI screening questionaire, the first part of which is here.
As part of my own research, I have been that guy asking the questions (in a slightly different context). At some point I'll write about this in more detail, but suffice to say that it's hard to trying to retrospectively diagnose mental illness in someone you've never met before. The potential for denial, mis-remembering, malingering, forgetting or just plain failure to understand the questions is enormous, although it doesn't come across in the final data, which looks lovely and neat.
The authors of the JAMA paper are well aware of this which is why they're skeptical of the apparantly large cross-national differences. In fact, most of their comment section consists of caveats to that effect. Just a few (edited, emphasis mine - see the full paper for more, it's free):
An important limitation of the WMH surveys is their wide variation in response rate. In addition, some of the surveys had response rates below normally accepted standards [i.e. many people refused to participate]... performance of the WMH-CIDI could be worse in other parts of the world either because the concepts and phrases used to describe mental syndromes are less consonant with cultural concepts than in developed Western countries [almost certainly they are] or because absence of a tradition of free speech and anonymous public opinion surveying causes greater reluctance to admit emotional or substance-abuse problems than in developed Western countries. [again, almost certainly, and Europeans are generally more reserved than Americans in this regard.] ... some patterns in the data (e.g. the much lower estimated rate of alcoholism in Ukraine than expected from administrative data documenting an important role of alcoholism in mortality in that country) raise concerns about differential validity.There's another, more fundamental problem with this data. On any meaningful criterion of "mental illness", a society in which 25% people were mentally ill in any given year would probably collapse. The WHO survey, however, is based on the DSM-IV criteria of mental illness. These are are increasingly regarded as very broad; for example, DSM-IV does not distinguish between feeling miserable & down for two weeks because your boyfriend leaves you, and spending a month in bed hardly eating for no apparant reason. Both are classed as "depression", and hence a "mental illness", although 50 years ago, only the second would have been considered a disease. For someone who styles himself a rebel in the mould of R. D. Laing, it's baffling that James accepts the American Psychiatric Association's dubious criteria.
What other data could we look at? Ideally, we want a measure of mental illness which is meaningful, objective and unambigious. Well, there aren't any, but suicide rates might be the next best thing - they're nice hard numbers which are difficult to fudge (although in cultures in which suicide is strongly taboo, suicides may be reported as deaths from other causes.) Although not everyone who commits suicide is mentally ill, it is fair to say that if Britain really were twice as unhappy as the rest of Europe, we would have a relatively high suicide rate.
What's the data? Well, according to Chishti et. al. (2003) Suicide Mortality in the European Union, we don't.
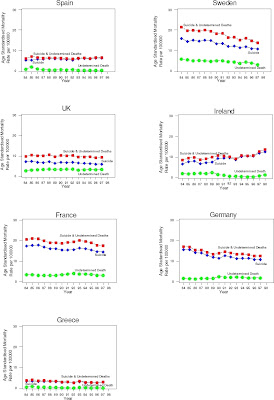 In fact suicide rates in the UK are boringly middle of the road. They're higher than in places like Greece and Spain, but well below rates in France, Sweden and Germany. Suicide rates are not a direct measure of rates of mental illness, because not everyone who commits suicide is mentally ill, and the rate of succesful suicide depends upon access to lethal means. But does this data look compatible with James's claim that rates of "mental illness" are twice as high in Britain as on "the Continent"? - or indeed with James's implicit assumption that "the Continent" is monolithic?
In fact suicide rates in the UK are boringly middle of the road. They're higher than in places like Greece and Spain, but well below rates in France, Sweden and Germany. Suicide rates are not a direct measure of rates of mental illness, because not everyone who commits suicide is mentally ill, and the rate of succesful suicide depends upon access to lethal means. But does this data look compatible with James's claim that rates of "mental illness" are twice as high in Britain as on "the Continent"? - or indeed with James's implicit assumption that "the Continent" is monolithic?What's odd is that James clearly knows a bit about suicide, or at least he does now, because just today he wrote a remarkably sensible article about suicide statistics for the Guardian. So he really ought to know better.
Drug sales are another nice, hard number. Of course, medication rates do not equal illness rates - in any field of medicine, but especially psychiatry. Doctors in some countries may be more willing to use drugs, or patients may be more willing to take them. With that in mind, the fact that population-adjusted (source, also here) British sales of antidepressants drugs are twice those of Ireland and Italy, equal to those of Spain, and half those of France, Norway and Sweden does not necessarily mean very much. But it hardly supports James's theory either.
Interestingly, although James holds up Denmark as an example of the kind of happy, "unselfish capitalism" that we should aspire to, the Danes take 50% more antidepressants than we do! (They also have a much higher suicide rate.) True, sales of anxiety drugs and sleeping pills are relatively high in the UK, but still less than Denmark's. Most interestingly, sales of antipsychotics are very low in the UK - roughly the same as in Germany and Italy but less than a quarter of the sales in Ireland and Finland!
So cheer up, Anglos. We're not twice as sad as the French. More likely, we are just more open about talking our problems in the interests of scientific research. However, the French, to their credit, didn't give the world Oliver James.
[BPSDB]
(*) This is Oliver James, psychologist. Not to be confused with: Oliver James, heartthrob actor; Oliver James, Fleet Foxes song, and Oliver James, Ltd.
 Posted in
bad neuroscience,
books,
media,
mental health,
oliver james,
papers
Posted in
bad neuroscience,
books,
media,
mental health,
oliver james,
papers

